IDENTIFYING AND ANALYZING RISK
Our research and development team consists of leading experts in the area of program evaluation analysis and performance assessment. Our analytics and reporting package assimilates available health and financial data sources into one powerful and central resource to facilitate more informed and strategic decision making. Reports are available in multiple areas of plan management, including claims and cost analysis, risk identification, risk modeling, plan performance and plan modeling, and Return on Investment (ROI).
|
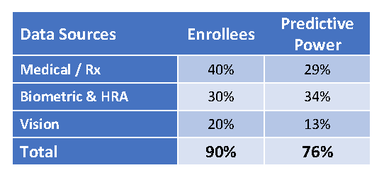
Consider this - 30% of employees will have no medical or Rx claims this year and another 30% will have so few claims that their data will have very little value. Yet, it's very possible that these people will account for a significant portion of next year's claims cost. Insurance carriers and pharmacy benefit managers alone produce a mere 29% accuracy when predicting who will need costly medical care within the next 12 months. Through a proprietary analytics engine, vetted by analysis of more than 11 million members, we provide predictive modeling analysis with a predictive accuracy up to 76%. The unique capability we provide through our analytics engine is achieved by consolidating data that otherwise is housed in separate arenas. This analysis enables forecasting of future health costs and identifies individual areas of risk allowing for proactive engagement.
|
REPORTING AND MANAGING
The unique power of the analytics we perform allow us to identify individuals currently at risk as well as those with a high future health risk. Our identification process includes those without claims that otherwise appear healthy. Our clinicians are trained to pinpoint the appropriate level of intervention whether it be a health coach, nurse care management, disease management, or prescription formulary intervention. In addition, we are uniquely positioned to recognize gaps in care and offer recommendations for appropriate treatment.